The discovery of penicillin in 1928 is considered one of the most important developments in the history of modern medicine. Since their inception antibiotics have without a doubt saved many lives by helping people to overcome serious infections. However, today according to health authorities they are being overprescribed, with estimates ranging from 20% to 50% being deemed as inappropriate. This is a worrying trend because the overuse of antibiotics for non-life threatening conditions, and their use as growth promoters for conventionally farmed livestock, has contributed greatly to gut dysbiosis (microbial imbalance that detrimentally impacts on normal bodily function), pathogen colonization of the gut, pathogen evolution, and the downward spiral of general human health in ways that are as yet not fully understood.
A recent study published in the journal Cell Host and Microbe (Rivera-Chávez et al., 2016) however, sheds new light on some of the processes going on in the dark recesses of the 300 – 400 m2 area of the human gastrointestinal (GI) tract when we are exposed to antibiotics. The study, led by Andreas Bäumler, professor of medical immunology and microbiology at UC Davis Health System, sought to uncover the mechanisms by which antibiotic treatment effect changes in the gut that allow the proliferation of pathogenic bacteria. While the healthy human GI tract houses a microbial community that prevents pathogen dominance through largely unknown mechanisms, antibiotic treatment is known to increase susceptibility to enteric (gut) pathogens. The question Bäumler and his team asked was, “how?”
“The road to health is paved with good intestines!”
Sherry A. Rogers
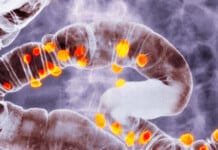
The healthy human gut is a largely anaerobic (oxygen free) environment, and beneficial bacteria that support human health such as those in the class Clostridia thrive in low oxygen conditions. Meanwhile, pathogens such as Salmonella that have the capacity to compromise our health, flourish in an oxygen rich environment, and are inhibited by its lack.
Bäumler and his team focused on the Clostridia/Salmonella balance and soon discovered that the move away from optimal balance in the gut begins when antibiotics kill the “good” guys along with the “bad”.
Many species in the Clostridia class consume dietary fibre (a ‘prebiotic’, that provides food for probiotic bacteria) to create a range of metabolites essential to gut health and integrity, including butyrate. Butyrate is a short chain fatty-acid utilised by the cells of the colon as an energy source, allowing them to absorb water. Lack of butyrate initiates autophagy (self-digestion) in these cells, and in extreme cases, these cells die. Decreased intestinal metabolism results in an increase in local oxygen concentrations, which favours pathogenic oxygen-loving organisms. According to Bäumler, “Salmonella flourished in the newly created oxygen-rich micro environment after antibiotic treatment. In essence, antibiotics enabled pathogens in the gut to breathe.”
Unfortunately, we don’t just get antibiotics from the doctor.
Low-dose antibiotics are used to improve weight gain in livestock, and human consumption of meat and animal products thusly treated has been linked to a host of health issues, including the modern obesity epidemic.
On the other side of the imbalance coin, we find that routes for probiotic species to enter the body are compromised by: modern agricultural practices which kill beneficial bacterial species on produce (for example, glyphosate is a powerful antimicrobial agent); diets overly reliant on processed rather than fresh ‘chemical free’ foods; the ‘war on germs’; pasteurisation; and reduced consumption of fermented foods compared to previous generations.
Gut dysbiosis combined with antibiotic use has one more trick up its sleeve though – bacteria not only have rapid generational turnover (an estimated 20 minutes for GI tract bacteria), they also engage in ‘horizontal’ gene transfer, which means they can swap genetic material.
In an imbalanced gut, as pathogens gain dominance, evolution of traits such as antibiotic resistance can be very rapid indeed, and once established, this trait may be passed horizontally not only within species, but between species.
”All disease begins in the gut.:
Hippocrates
Gut dysbiosis at its most simple is an imbalance within the community of bacteria in the GI tract. Most telling in a clinical context is the ratio between the bacterial phyla Firmicutes and Bacteroidetes (F/B ratio), but since gut dysbiosis also favours the Proteobacteria, their overgrowth often co-occurs with Bacteroidetes dominance.
Dominance of Bacteroidetes is associated with a host of health problems including obesity, hypertension, depression, IBS, Crohn’s disease, autism, type 1 and 2 diabetes, multiple sclerosis, and many other auto-immune conditions, while the phylum Proteobacteria contains well known pathogens in genera such as Salmonella, Escherichia, and Helicobacter.
There are many factors other than antibiotics that can cause imbalance of the F/B ratio, including diet, infection, environmental toxins, neurotoxins, and chronic systemic inflammation. And just like the chicken and the egg, either gut dysbiosis or bodily dysfunction may occur first and be the cause of the other, and the addressing or healing of one can have a positive effect on the other.
What we soon find though upon a thorough investigation of gut dysbiosis and subsequent human dysfunction is that we are far from having a full understanding of the mechanisms involved, and these mechanisms are so diverse and interrelated that a broad-based, holistic, and natural approach is our best bet for maintaining a healthy gut.
What can we do to encourage and maintain balance within our internal ecosystem of micro-organisms?
From the little we do know, the following procedures will be beneficial:
Be careful with antibiotics:
Antibiotics can be a life-saving intervention, but we should reserve their use for serious infections. Over or inappropriate use (e.g. taking antibiotics for a low grade or a viral infection) encourages gut dysbiosis, and facilitates the evolution of antibiotic resistant bacterial strains. Try natural antibiotics such as garlic, cat’s claw tea or oregano oil.
Eat well:
Nutrient dense, fresh, clean, local, and seasonal food with a high component of raw greens and adequate dietary fibre is best for the gut. Consider eliminating foods that trigger inflammation in the body, these foods can be different for each of us, but eliminating or restricting sugar and gluten is a good start for most.
Avoid low-dose antibiotic treated animal products:
Research indicates multiple problems with these foods. Try to eat only organic animal products, and consider reducing the amount eaten.
Avoid environmental, dietary, and other toxins:
Many toxins initiate chronic inflammation, and researching things such as food additives, fluoridation, heavy vaccination schedules, plastics, and electromagnetic exposure will help you make up your own mind about what you should avoid or limit.
Consume beneficial organisms:
A regular supply of good bacteria either through probiotic supplementation, or even better, a diversity of fermented foods, will greatly help in maintaining a healthy balance in the gut.
Reduce stress:
The effects of cortisol on every bodily system are so profound, stress reduction should really be taught in schools. Find what suits you best to reduce stress, whether it be meditation, yoga, a walk in nature, a swim, conversation with good friends, or anything that relaxes you.